DISCUSSION
The skin is the major barrier between the internal environment of the body and the external environment's hazards. The epidermal layer is "disposable," in the sense that its very rapid rate of production of new cells can make up for significant loss to abrasion, injury, etc. It has a considerable, but finite, capacity for immediate repair.
 The skin is a "target" for exoparasites. Fleas and ticks have developed ways to get past the thin epidermal layer (especially that of the flanks and abdomen, which is why it typically is localized to these areas); they can easily pierce it with their blood-sucking apparatus to access the rich network of blood vessels in the dermis. Systemic exposure to allergens is pretty much inevitable as the fleas take a blood meal.
The skin is a "target" for exoparasites. Fleas and ticks have developed ways to get past the thin epidermal layer (especially that of the flanks and abdomen, which is why it typically is localized to these areas); they can easily pierce it with their blood-sucking apparatus to access the rich network of blood vessels in the dermis. Systemic exposure to allergens is pretty much inevitable as the fleas take a blood meal.
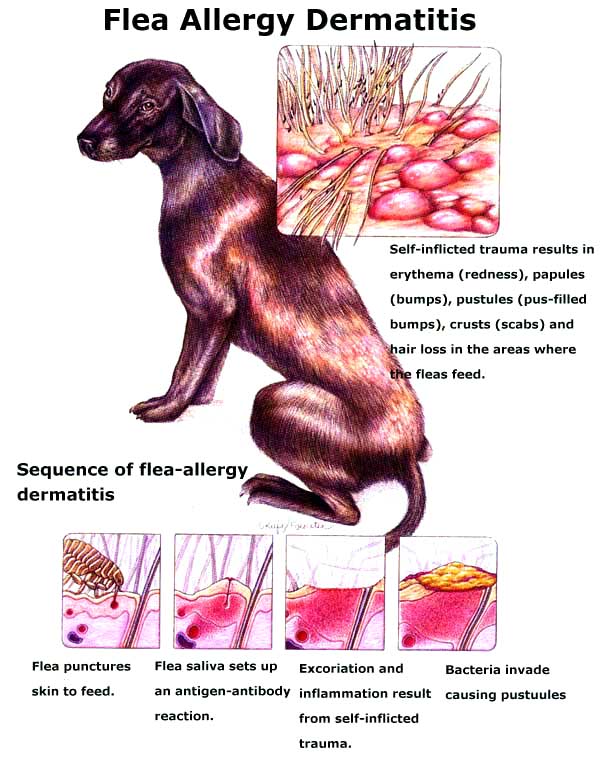 If hypersensitivity develops, the tissue damage associated with inflammation may become too great even for the skin to repair and opportunistic infections with common bacteria (principally Staphylococcus
If hypersensitivity develops, the tissue damage associated with inflammation may become too great even for the skin to repair and opportunistic infections with common bacteria (principally Staphylococcus ![]() intermedius and Malassezia
intermedius and Malassezia ![]() pachydermatis) can gain a foothold.
pachydermatis) can gain a foothold. ![]()
![]() Chronic itching and scratching causes affected areas become alopecic,
Chronic itching and scratching causes affected areas become alopecic, ![]() lichenified, and hyperpigmented. Hair is affected because it, too, is part of the epidermis.
lichenified, and hyperpigmented. Hair is affected because it, too, is part of the epidermis.
So flea allergy dermatitis begins with flea saliva, which ![]() contains numerous antigenic materials: amino acids, aromatic
contains numerous antigenic materials: amino acids, aromatic ![]() compounds, polypeptides, and
compounds, polypeptides, and ![]() phosphorus. These
phosphorus. These ![]() substances have
substances have ![]() molecular weights between 18,000 to
molecular weights between 18,000 to ![]() 45,000 daltons with the major
45,000 daltons with the major ![]() allergen of MW 30,000 to
allergen of MW 30,000 to ![]() 32,000 daltons. Dogs present with a history of severe scratching, chewing, licking,
32,000 daltons. Dogs present with a history of severe scratching, chewing, licking, ![]() biting, and other signs of pruritus. The owners don't really pay too much attention to a dog's scratching unless it gets excessive and the damage is obvious.
biting, and other signs of pruritus. The owners don't really pay too much attention to a dog's scratching unless it gets excessive and the damage is obvious.
 Sixty-one percent of flea-allergic
Sixty-one percent of flea-allergic ![]() dogs develop clinical signs
dogs develop clinical signs ![]() between 1 and 3 years of age. With age and continued
between 1 and 3 years of age. With age and continued ![]() exposure to fleas, the degree of
exposure to fleas, the degree of ![]() hypersensitivity may wane. FAD
hypersensitivity may wane. FAD ![]() is uncommon in dogs less than 6
is uncommon in dogs less than 6 ![]() months of age because their immune systems are not yet fully competent. Many
months of age because their immune systems are not yet fully competent. Many ![]() dogs who are allergic to the bite
dogs who are allergic to the bite ![]() of a flea have very few fleas on
of a flea have very few fleas on ![]() them at any time because their
them at any time because their ![]() excessive grooming activity
excessive grooming activity ![]() removes the fleas.
removes the fleas.
 Patients usually
Patients usually ![]() have papules, crusts, salivary
have papules, crusts, salivary ![]() stains, excoriations, and
stains, excoriations, and ![]() erythema in a wedge-shaped
erythema in a wedge-shaped ![]() pattern over the lumbosacral
pattern over the lumbosacral ![]() region, caudal thighs, proximal
region, caudal thighs, proximal ![]() tail, ventral abdomen, and around
tail, ventral abdomen, and around ![]() the umbilicus. FAD can be diagnosed based on age at onset of symptoms, distribution of the pruritus and
the umbilicus. FAD can be diagnosed based on age at onset of symptoms, distribution of the pruritus and ![]() clinical signs, and the observation
clinical signs, and the observation ![]() of fleas and/or flea feces.
of fleas and/or flea feces.
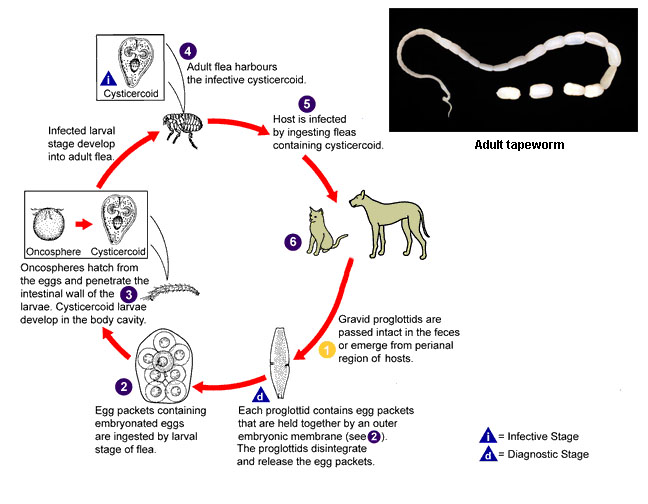
Many dogs affected by flea dermatitis will have recurrent ![]() tapeworm (Diplydium
tapeworm (Diplydium ![]() caninum) infestations from
caninum) infestations from ![]() ingestion of the fleas. The
ingestion of the fleas. The ![]() diagnosis of FAD can be
diagnosis of FAD can be ![]() confirmed with an intradermal
confirmed with an intradermal ![]() skin test with flea antigen.
skin test with flea antigen. ![]()

 Therapy for the allergic reaction is based on the severity and history of the symptoms: it may include topical treatments, medicated shampoos, steroids, antihistamines, antibiotics, and fatty acid supplements such as skin oil replacement. The effectiveness of allergy shots, or hyposensitization, for treating flea bite hypersensitivity remains controversial. While symptomatic relief can be provided, the only real "treatment" for a dog with this condition is to keep him flea-free if possible. This requires some understanding of the flea life cycle.
Therapy for the allergic reaction is based on the severity and history of the symptoms: it may include topical treatments, medicated shampoos, steroids, antihistamines, antibiotics, and fatty acid supplements such as skin oil replacement. The effectiveness of allergy shots, or hyposensitization, for treating flea bite hypersensitivity remains controversial. While symptomatic relief can be provided, the only real "treatment" for a dog with this condition is to keep him flea-free if possible. This requires some understanding of the flea life cycle.
Fleas don't breed on the dog: they deposit their eggs in bedding and nearby objects. The larval fleas aren't on the dog, they're in his environment. While flea-killing agents work on the dog, it's also necessary to kill all the life stages, which means treating the dog's environment. Yard sprays, house foggers, regular washing or changing of bedding will all help keep the flea population in check. The owners need to be educated about flea control methods as much as anything else.